Meet the George Mason senior changing breast cancer research
Katarina Benson
In January, George Mason University senior Angela Victoria Rojas Rivera represented the university at the National Collegiate Research Conference (NCRC). Led and hosted by Harvard University, NCRC is the largest student-run research conference in the United States. Only 200 students are selected to attend.
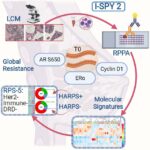
Rojas Rivera’s project “Extracellular Vesicle–Driven Immune Programming at the Sentinel Lymph Node in Triple-Negative Breast Cancer” found a new immunotherapy approach that helps the body recognize breast cancer cells as a threat, allowing the immune system to respond faster.

“By changing the cancer’s messages, this localized immunotherapy helps the immune system respond earlier and more effectively, offering a promising strategy to prevent cancer from spreading while reducing side effects,” she explained.
After presenting her earlier findings at the Network for Undergraduate Research in Virginia (NURVa) poster event last year, Rojas Rivera has continued to work on her research at George Mason’s Center for Applied Proteomics and Molecular Medicine (CAPMM) with her mentors Lance Liotta and Marissa Howard. After graduation, Rojas Rivera plans to pursue a PhD in biomedicine or proteomics.
“I am deeply committed to developing this research into a real, effective treatment,” she said.
From a student with no prior research experience to a confident scholar with deep expertise, Angela has become a force within George Mason’s research community,” said Liotta, who is co-director of CAPMM. “Her excellence extends far beyond the lab. By representing the university at the NCRC, Angela elevated not only her own voice but also the visibility of George Mason and the College of Science.”
Rojas Rivera is also one of only four students admitted to the highly selective histology program at Inova Hospital, a full-time, 10-month (40-week) training program designed to prepare current university students for careers as certified histotechnologists. She credits her mentors and Office of Student Creative Activities and Research (OSCAR) for allowing her to stand out as a candidate.
“George Mason offers strong access to research opportunities, particularly through funding programs like OSCAR and faculty mentorship, which make it easier for undergraduates to become involved in meaningful research,” she said. “That kind of support plays an important role in helping students take research seriously and pursue it beyond the classroom.”
Asked about her advice for undergraduates who’d like to take the next step in their research career, Rojas Rivera said: “Don’t overthink it—just do it. Even as undergraduates, our work has value and taking that first step can shape not only our careers, but the future of science itself.”